Spinal bifida, a congenital disorder, 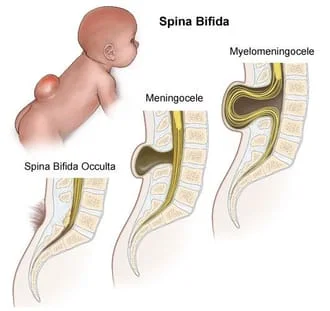
Spina bifida is a neural tube defect. The neural tube, during development, is a structure in the embryo that becomes the brain and spinal cord (and their enclosing tissues). The neural tube is supposed to close within 28 days of conception. If it does not close properly, spinal cord and backbone defects occur.1 One way to prevent 70% of the spina bifida cases is to take 400 mcg of folic acid every day, before becoming pregnant. Those women with a family history, or prior pregnancy resulting in this disorder, should consider higher doses of folic acid with their caregiver.2 Spina bifida means, literally, “open spine”. While it is suggested that there are some genes involved, other possible causes include high fever during pregnancy, or use of the epileptic medication, valproic acid.
Spina bifida has two forms. Spina bifida occulta, the mildest form, means that the defect is “hidden” by skin. There may not be symptoms, and the spinal cord may not be affected. Spina bifida manifesta can involve the meninges (“meningocele”), which protect the brain and spinal cord. The most severe spina bifida manifesta is called “myelomeningocele”, when the meninges and spinal cord actually “push through the hole in the back”. Most of these affected babies have fluid around the brain, or hydrocephalus, as well. Paralysis, to some degree, is typically another result of this disorder. The higher on the back that the opening is, the more severe the paralysis is. Other complications of spina bifida include bladder and bowel control problems, attention deficit hyperactivity disorder (ADHD), hand-eye coordination problems, and learning difficulties.3 Additional issues resulting from spinal bifida may include pressure sores, abnormal eye movement, club foot, scoliosis, hip dislocation, leg weakness, brain abnormalities, poor cognitive flexibility, difficulty planning and organizing, and social troubles. Most children with spina bifida also develop latex allergies, which can make medical treatments more challenging (due to its presence in catheters and gloves).4
Traditional Treatments
Spina bifida may require surgery. The hole can be closed, but that won’t restore spinal cord functionality. There are investigations into the safety and efficacy of intrauterine surgery (performed before birth), but the most effective thing to do is to prevent spina bifida by taking folic acid before pregnancy. There is no cure for the nerve damage caused by this disease. A surgically inserted shunt can help drain the cerebrospinal fluid, the abdomen, or the chest. Many medically based teams work together to help patients cope with spina bifida, such as: physiatrists, orthopedists, neurosurgeons, neurologists, urologists, ophthalmologists, physical therapists, occupational therapists, speech therapists, and psychologists. Orthotists can design “assistive technology”, such as braces, wheelchairs, walkers, and crutches.5 Obesity can be a problem in people with spina bifida, and this could affect daily living and put patients at risk of other diseases. Exercise and healthy eating can prevent obesity.6
Alternatives
A case study of a young body with bowel and urinary incontinence showed the promise of chiropractic care. The chiropractor used the Activator and shortwave diathermy over several treatments, and the patient achieved “satisfactory bladder and bowel control”.7 It is not uncommon for patients to seek chiropractic and massage care. These can be very safe therapies, as long as certain precautions are taken to protect the patient. Practitioners should be careful around shunts, avoid rapid head twists, and be aware of applying too much pressure to certain regions.8
References:
1 http://www.mayoclinic.com/health/spina-bifida/DS00417
2 http://www.spinabifidaassociation.org/site/c.evKRI7OXIoJ8H/b.8029671/k.8354/Why_Folic_Acid.htm
3 http://kidshealth.org/parent/system/ill/spina_bifida.html
4, 5 http://en.wikipedia.org/wiki/Spina_bifida
7 http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3081241/
6,8 http://www.kintera.org/site/c.liKWL7PLLrF/b.3077279/k.59D2/FAQ_about_Spina_Bifida.htm

